I’m writing as a husband trying to help other men understand what endometriosis really means for the women we love. My wife lives with advanced stage IV deep endometriosis (and fibromyalgia), and I’ve spent countless hours, weeks, years researching her symptoms.
Every story she tells (about doctors, symptoms, or how she feels on a bad day) drives me to learn more.
I’m not a doctor. I’m just a husband who refuses to give up! What I’m sharing here is the result of that journey and of listening to many women’s experiences. Your lived truth matters most. If I make mistakes or oversimplify anything, please correct me. I want to be as accurate and helpful as possible.
Most people still think endometriosis is “just bad periods” and only affects the uterus and ovaries. In fact, endo affects roughly 5–10% of reproductive-age women worldwide. That’s tens of millions of women in the US and EU alone. Some experts even estimate about 1 in 9 women in the US (≈11%), and 1 in 9 women in the Australia have endo.
Equally shocking, diagnosis is often years late, on average 4–11 years from first symptoms. Many women see multiple doctors (some studies found nearly half see 5+ physicians) before anyone connects the dots. So when she’s suffered silently for so long, it’s no wonder she’s frustrated by dismissals like “it’s just anxiety.”
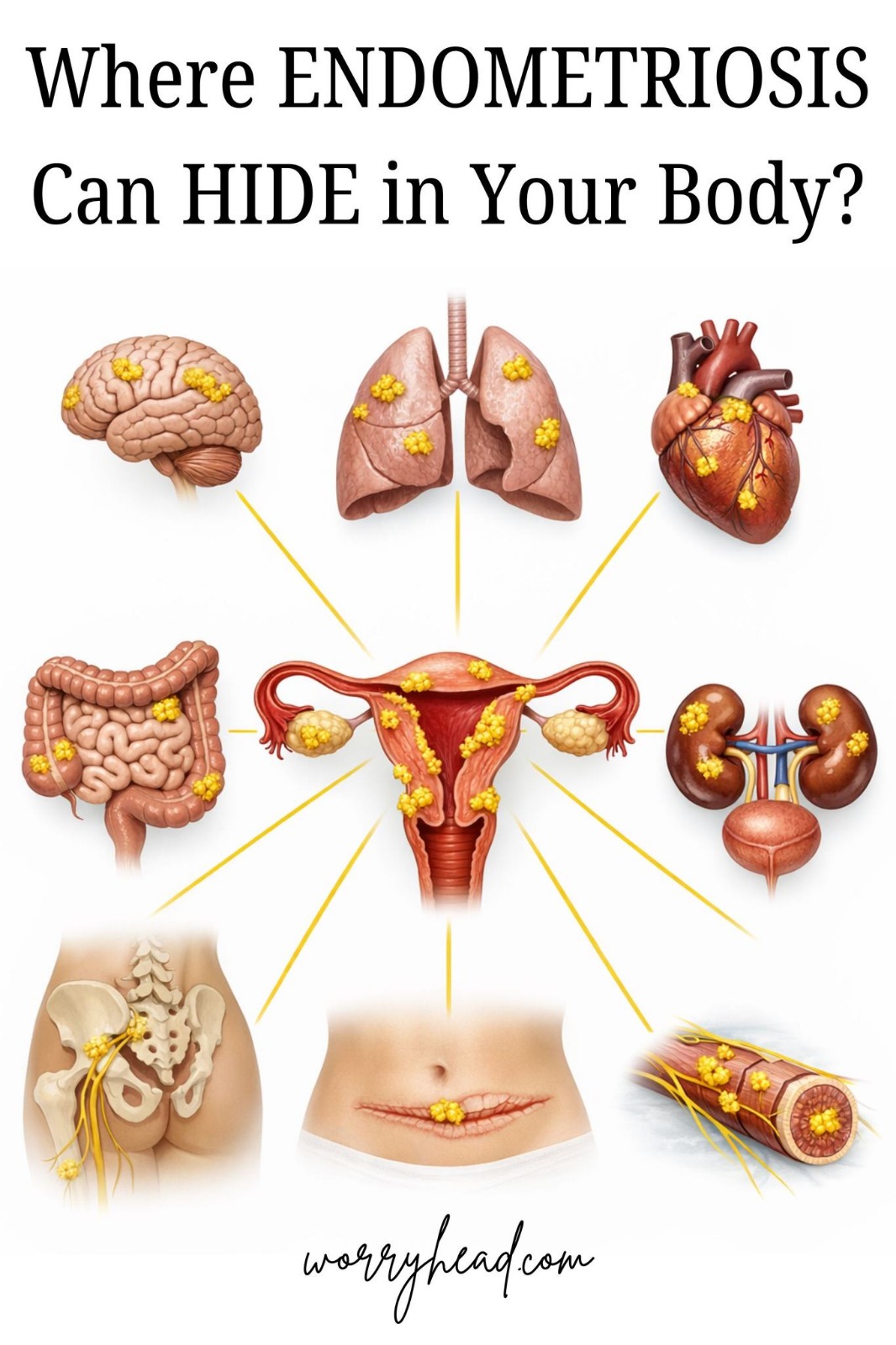
Endometriosis is increasingly recognized as a systemic, chronic inflammatory disease, not just a “uterine problem”.
The classic definition is “endometrial-like tissue outside the uterus”, but modern research shows it often behaves like a body-wide illness.
Endo tissue is still hormonally active and bleeds each month, causing inflammation wherever it implants. It runs in families (genes matter) and is linked to immune dysregulation: many women with endo also have other autoimmune issues (thyroid disease, lupus, etc.). Blood and lymphatic spread can carry endo cells far from the pelvis.
Over time, repeated cycles of bleeding and healing create scar tissue (adhesions) that glue organs together. This means endo tends to worsen or spread over time, so it requires long-term, multidisciplinary care (surgery/hormones plus pain management, nutrition, physical therapy, and mental health support).
In short, this disease is life-shaping, not just inconvenient!
It can mean crippling pain every month (and often between periods), heavy fatigue, digestive and bladder problems, and serious fertility struggles. For example, endo is found in up to 50% of otherwise-unexplained infertility cases.
Endo causes chronic inflammation throughout the body and even reprograms the brain’s pain and hormone signaling. It raises long-term risks for conditions like heart disease and stroke on top ofvthus diabolical already disease.
Imagine coping with that, and then not being believed when you’re hurting… That’s why partners need to listen!
What Is endometriosis, really?
Medically, endometriosis is defined as endometrial-like tissue growing outside the uterus. The “textbook” locations are the ovaries (creating chocolate cysts), fallopian tubes, and peritoneal lining of the pelvis.
These explain classic symptoms: agonizing menstrual cramps (dysmenorrhea), chronic pelvic pain, pain during sex, and infertility. Indeed, about half of women with unexplained infertility have endo.
But that definition barely scratches the surface. We now know:
• Retrograde flow is NOT enough: Sampson’s theory of backward menstrual flow through the tubes explains some cases, but not all. Endometriosis can spread via blood or lymphatic channels. In fact, pathologists have found endometrial cells in pelvic lymph nodes and even the brain, proving these cells can ride the circulation and implant far from the uterus.
• Hormones & genetics: Endo is strongly driven by estrogen. Women with early menarche, late menopause, or long estrogen therapy have more risk. There’s a clear genetic component, if your mother or sister has it, your risk is higher. But hormones alone don’t explain everything.
• Immune/inflammatory disease: Women with endo often show altered immune function. Their bodies act as if the displaced tissue should just stay (instead of attacking it). This is why many researchers now think of endo alongside autoimmune conditions. For example, Petraglia et al. note that endo frequently overlaps with other inflammatory diseases, suggesting an immune-system malfunction. If she also has thyroid problems, allergies, or fibromyalgia (a common overlap), those aren’t “coincidences”, they’re pieces of a systemic puzzle.
Read more on next page
ADVERTISEMENT
ADVERTISEMENT