ADVERTISEMENT
ADVERTISEMENT
Endometriosis: a whole-body, whole-life struggle…
• Chronic & progressing: Endometriosis often behaves like a chronic wound. Each month the implants bleed, tissue fibrin is laid down, adhesions form between organs, and new pain pathways develop. Over time, this can distort anatomy (e.g. dragging ovaries into funny positions). Surgeons often find dense scar tissue after years of untreated endo. Even after surgical removal of lesions, the disease can recur and new lesions can develop, which is why ongoing management is needed.
• Whole-person approach: Modern guidelines stress that endo care must be multidisciplinary. Surgery or hormonal pills alone often aren’t enough. Many women benefit from pelvic floor physical therapy, nutritional changes (to reduce inflammation), pain neuromodulators, and psychological support. As partners, we become part of that support network when we learn to validate her pain and assist with holistic care.
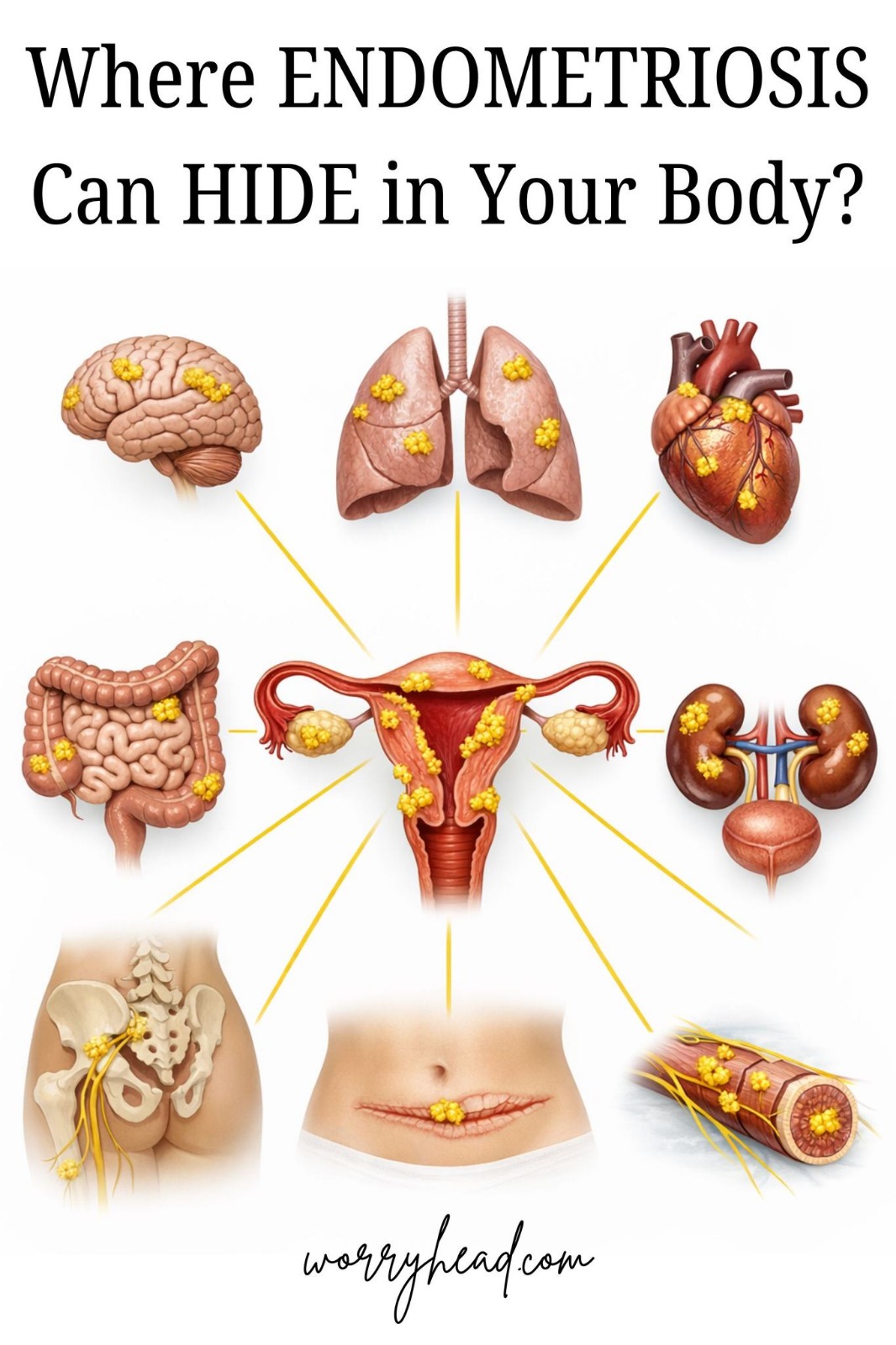
Endometriosis is not just a pelvic condition, but a multi-system disease with neurological and immunological involvement. That’s why its nickname “the silent pandemic” is fitting. It quietly affects all aspects of life.
What arevthe symptoms & signs beyond the periods?
Yes, endo typically causes very painful periods (called dysmenorrhea) and pelvic pain. Many women describe cramping so intense it’s like being stabbed or burned with heat.
About 50–75% of women with endo have pain during sex (dyspareunia). Over-the-counter meds often do not help enough – it frequently takes prescription narcotics, nerve blocks, or a heating pad and bedrest.
But endo can do so much more:
• Extremely painful periods: Dysmenorrhea is the hallmark. It usually starts at the very beginning of her bleeding and can last 3–7 days. Women often miss school or work because of it. Research consistently finds dysmenorrhea to be one of the most reliable symptoms of endo (even when imaging looks “normal”).
• Chronic pelvic/abdominal pain: Many women have persistent aches or sharp pains in the lower belly or back even between periods. This may be due to adhesions tugging on organs. It can feel like a dull ache or sudden stabbing. Chronic daily pain is common and can be debilitating.
• Heavy, irregular bleeding: The extra implants bleed on top of the normal uterine lining. This often causes menorrhagia (very heavy periods, large clots) or spotting between periods. If she’s anemic or always exhausted from bleeding, endo could be the unseen reason. (Some women also have adenomyosis, which worsens bleeding, but that is often comorbid with endo.)
• Digestive issues: Lesions on the intestines cause GI symptoms. This can include dyschezia (pain with bowel movements) especially during her period. She might have cyclical constipation or diarrhea, gas and bloating that resolve after menstruation, or even blood on the stool during menses. In one survey, about 12% of endo patients had bowel lesions. A related study found that up to 40% of women treated for “long-standing IBS” ultimately had endometriosis as the true cause. If she’s ever been told “you probably have IBS” but also has bad period pain, consider the connection.
• Urinary symptoms: Endo can hit the urinary tract (bladder, ureters). She might feel like she has bladder spasms or infections every month, urgent, burning peeing that mostly happens around her period. Doctors often initially treat this as interstitial cystitis or recurrent UTIs. The scary scenario is a ureteral implant: if a lesion wraps around a ureter, it can slowly block the kidney. Urologists warn that by the time swelling of the kidney (hydronephrosis) is seen on imaging, up to 50% of that kidney’s function may already be lost. It can happen “silently.” So any cyclical flank pain or kidney issues in a woman with endo deserves urgent attention.
• Fatigue & “endo brain”: Chronic pain and heavy bleeding cause relentless fatigue. More than 50% of women with endo report debilitating fatigue at times. Combined with anxiety and poor sleep, this can feel like a constant flu. Many patients also report “brain fog” (trouble concentrating or memory lapses) especially when in pain or on hormones. This cognitive side is real and often overlooked.
Read more on next page
ADVERTISEMENT